
In order to understand the goals of dialysis and why it is so crucial to the health of people with kidney failure, the function of healthy kidneys must be known.
The kidneys are the filtering devices of blood. The kidneys remove waste products from metabolism such as urea, uric acid, and creatinine by producing and secreting urine. Urine may also contain sulfate and phenol waste and excess sodium, potassium, and chloride ions. The kidneys help maintain homeostasis by regulating the concentration and volume of body fluids. For example, the amount of H+ and HCO3 - secreted by the kidneys controls the body's pH.

The working units of the kidneys are called nephrons. There are approximately 500,000 nephrons in each kidney. In the diagram above, the nephrons are located in the cortex (cortical nephrons) and medulla (juxtamedullary nephron). In a given minute, 1200 milliliters of blood flows through the kidneys (Cooney, 270).
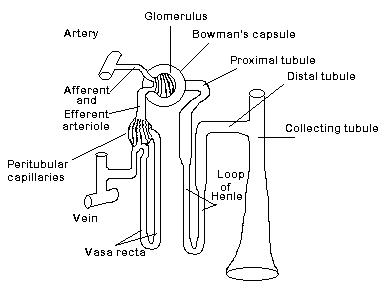
Blood flows into the kidneys through the renal artery and enters the glomerulus in Bowman's capsule. In the glomerulus, the blood flow is split into fifty capillaries that have very thin walls. The solutes in the blood are easily filtered through these walls due to the pressure gradient that exists between the blood in the capillaries and the fluid in the Bowman's capsule. The pressure gradient is controlled by the contraction or dilation of the arterioles. After passing through the afferent arteriole, the filtered blood enters the vasa recta. Blood exits the kidneys through the renal vein.
On the other hand, the particles and fluid removed from the blood, the filtrate, moves from the Bowman's capsule to the proximal tubule, loops of Henle, distal tubule, and collecting tubule. Urine is formed in the collecting duct and then exits through the ureter and bladder. From the proximal tube to the collecting tubule, the filtered blood and filtrate pass very close together. The peritubular capillaries (containing the filtered blood) are actually surrounded by the tubules. The nutrients that the body needs are reabsorbed into the blood at this point. Along with the nutrients that are reabsorbed into the blood, the balance of water and other molecules such as sodium and chloride is established by the reabsorption from the loop of Henle.
In the kidneys, active, passive, and osmotic transport are used to transfer molecules such as those mentioned above. The active transport of Na+ out of one side of the tubule membrane and into the peritubular capillaries creates an electrical potential inside the tubule and a concentration gradient between the tubule interior and membrane that causes Na+ to move from the interior through the membrane. This passive tranport causes another Na+ to enter the tubules on the opposite side due to the concentration gradient. Cl-, HCO3 -, and PO4 2- are also passively transported due to the electrical potential. Unlike those ions, H+ and K+ are actively secreted from the distal tubule and collecting duct. Water is osmotically transported. The osmotic shifts of water lead to diffusion of solutes between the tubules and capillaries. The amount of reabsorption of all the molecules depends on the concentrations in the tubules and in the peritubular capillaries. As well as the amount of the solute present, the amount that can be transported also depends on the permeabilities of the membranes for the particular solute. In general, wastes are poorly reabsorbed due to their lower membrane permeability, while the essential nutrients are more readily absorbed as their permeabilities are higher.
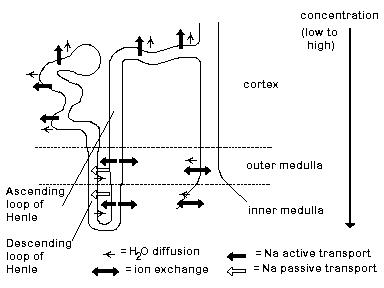
Because the human body does not maintain a constant water volume, the kidneys have to compensate for the lack of or excess of water consumed. The kidneys use a transport system called the counter-current mechanism to accomplish this (Hoppensteadt et al, 186). The name is based on the fact that concentration first increases in the direction of flow, then decreases as flow continues through the ascending parallel loop. The mechanism relies on the adjacent, parallel loops of Henle and vasa recta.
In the ascending loop, Na+ (or any solute) is actively pumped out of the tubule. As flow continues up the loop, the tubular concentration decreases as does the interstitial (the fluid surrounding the loop) concentration. Because water is impermeable in the ascending loop, the volume at the bottom of the loop is the same as that entering the distal tubule. At the bottom of the loop, the tubular and interstitial concentrations are equal.
In the descending loop, the concentrations inside and outside the tubule are increasing with the current, with the maximum concentration being reached at the bottom of the loop. The increased concentration is the result of the passive diffusion of Na+ into the tubule and water out of the tubule. When the filtrate reaches the distal tubule, a net loss of Na+ and water has occurred through the loops of Henle.
Inside the distal and collecting tubules, the filtrate is either diluted or concentrated to form urine. The regulating hormone for this process is ADH (antidiuretic hormone) and is excreted by the pituitary gland. The absence of ADH makes the membranes of the distal and collecting tubules impermeable to water. In this case, a larger volume of dilute urine is secreted. With ADH, water passively diffuses out of the tubules and a smaller volume of more concentrated urine results.
The maximum urine concentration is limited by the interstitial fluid concentration at the bottom of the loops of Henle. The urine leaving the collecting tubule has the same concentration as the interstitial fluid at that point. The interstitial concentrations are largely a function of blood flow in the three regions. In the cortex, the lower concentrations are the result of the large blood flow in the peritubular capillaries. The capillary blood carries away excess solute and water in the region. In the medulla, the only blood flow is in the vasa recta, approximately 10% of the cortical blood flow. The loop structure of the vasa recta keeps the entering and exiting concentration the same. While solute is absorbed in the descending loop, an equal amount of solute is secreted in the ascending loop.